"Mixing and matching" COVID-19 vaccines
Rachel Huang. 05/29/2021
The COVID-19 pandemic has lasted for over a year now, and many different brands of vaccines have been created in response to the coronavirus, such as the Pfizer-BioNTech, Moderna, Oxford-AstraZeneca and Johnson & Johnson vaccines. Even though not federally approved yet, the idea of mixing and matching these vaccines is gaining popularity as there is significant evidence that doing so strengthens the immune system. This “mix and match” method of administering vaccines can also be referred to as heterologous vaccination, which means that an individual receives one type of vaccine for their first shot and then another type for their second shot.
To better understand how this mixing approach utilizes different “types” of shots to strengthen the immune system, a brief overview of the human immune system is necessary. The human immune system has two main lines of defense: antibodies and T cells. Antibodies are proteins made by the immune system that bind to virus particles and “deactivate” them before they can infect any cells. T cells get rid of cells that have already been infected.
Most vaccines currently focus on the antibody line of the immune system and something on the coronavirus’ surface called a spike protein. The spike protein is what defines the coronavirus, so if your body is able to recognize the spike protein, it is able to recognize the coronavirus. The Pfizer and Moderna vaccines deliver mRNA, a set of instructions for the cell, to the ribosomes, where the cells can then recreate the spike protein. After the spike protein is completed, the body is able to recognize that the spike protein is a foreign object and starts building up a memory-like response to it with antibodies. On the other hand, Johnson & Johnson and Oxford-AstraZeneca notify the cell about the coronavirus’ spike protein by delivering another virus (an adenovirus) that has the spike protein “hidden” on it. The problem with using this Trojan horse-like contraption is that the immune system builds up immunity to the delivery molecule, in this case the adenovirus, which means that subsequent vaccinations will be less effective. Regardless of how they transfer the spike protein to our immune systems and the relative efficacy of their methods, the Pfizer, Moderna, Johnson & Johnson and Astra-Zeneca vaccines all protect our immune systems from their coronavirus by focusing on getting our cells to recognize the coronavirus’ spike protein.
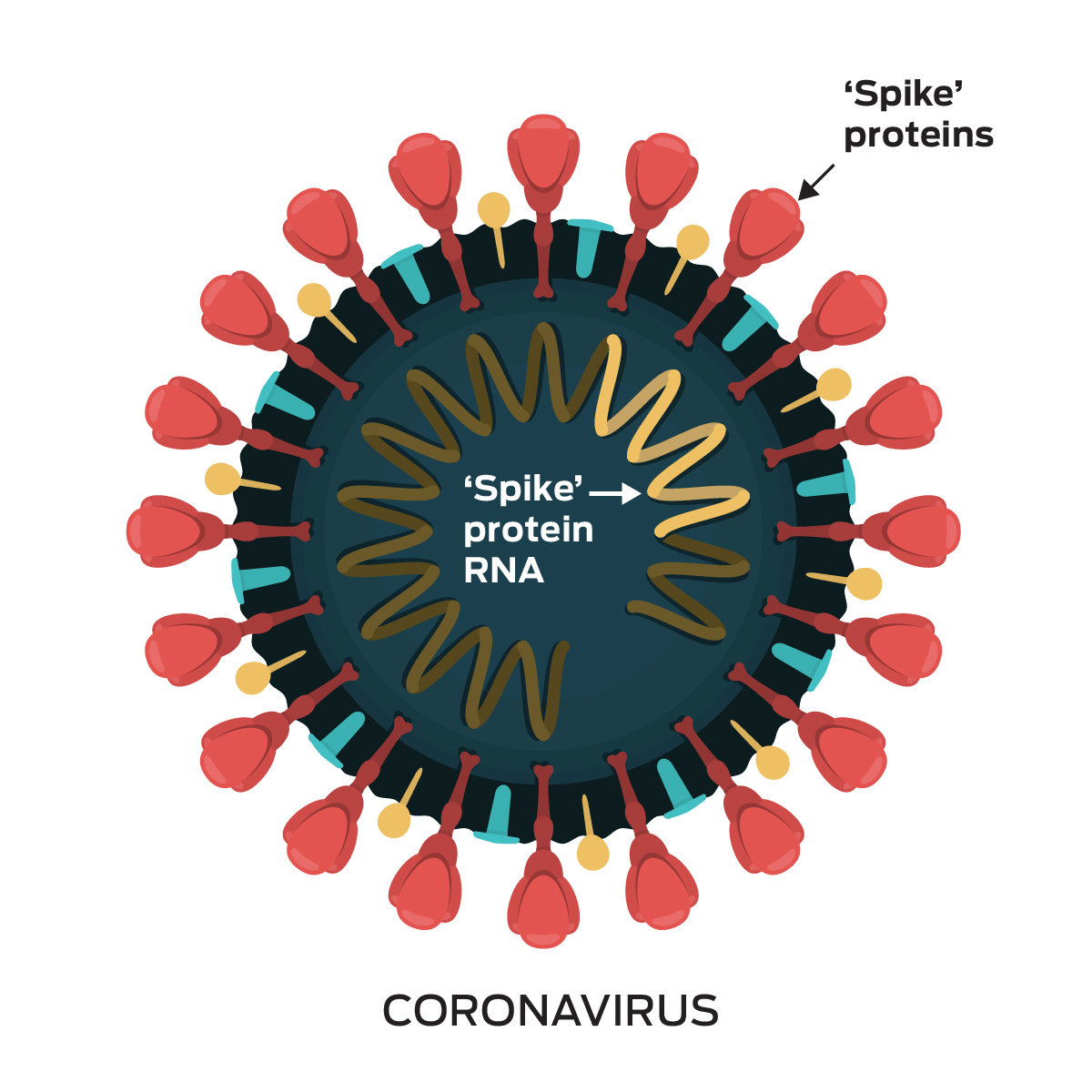
The problem with focusing on the spike protein is that viruses are constantly changing through mutation, and there are at least five variants of the coronavirus in the United States right now with modified spike proteins that may be unrecognizable to current vaccines. Here, the “mix and match” approach to administering vaccines comes into play, where Professor Shan Lu, the pioneer of this strategy, says that the mechanism of combining shots is where the first shot a person receives addresses the spike protein via antibodies, while the second shot rallies your T cells. Current plans to get the T cells’ “attention” center around adding another protein to the coronavirus, or using one that is already present like a nucleoprotein to boost T cell response. This additional protein will act as a name tag that T cells will be better able to recognize and respond to, increasing the number of T cells and antibodies in the cell due to the increased number of targets on the coronavirus. Together, T cells and antibodies will double the efficacy of our immune systems.
The United States, China, the United Kingdom, Spain and Russia have already begun human trials testing this mix and match method where participants receive the first dose of say, Pfizer, and then the second shot of Moderna. Gritstone, a company in California, has made it its mission to design two different vaccines that are made to be given together, instead of using two different brands of vaccines. Gritstone’s CEO, Andrew Allen, says that their approach may be able to “give recipients the best of both worlds [antibodies and T cells]!” and Phase 1 human clinical trials have also recently begun.
This mix and match method of administering vaccines is especially appealing from a scientific standpoint, especially for lower income countries that have less accessibility to vaccines. With heterologous vaccination, these countries will be able to continue administering vaccines even if one vaccine’s supply runs low or health concerns about a brand of vaccine arise. For people who worry about the safety of combining shots, “there is no danger in mixing vaccines,” Professor of Immunology at London School of Hygiene and Tropical medicine Helen Fletcher said. In fact, it may be more beneficial for patients with other diseases like MS and cancer whose antibody aspect of their immune systems have been weakened by their treatments. With bountiful scientific evidence proving that “mixing and matching” vaccines is beneficial for our immune systems, we can only hope that global and national authorities will quickly approve this strategy in order to strengthen us in our united fight against COVID-19.
Cover Photo: (NBC)
